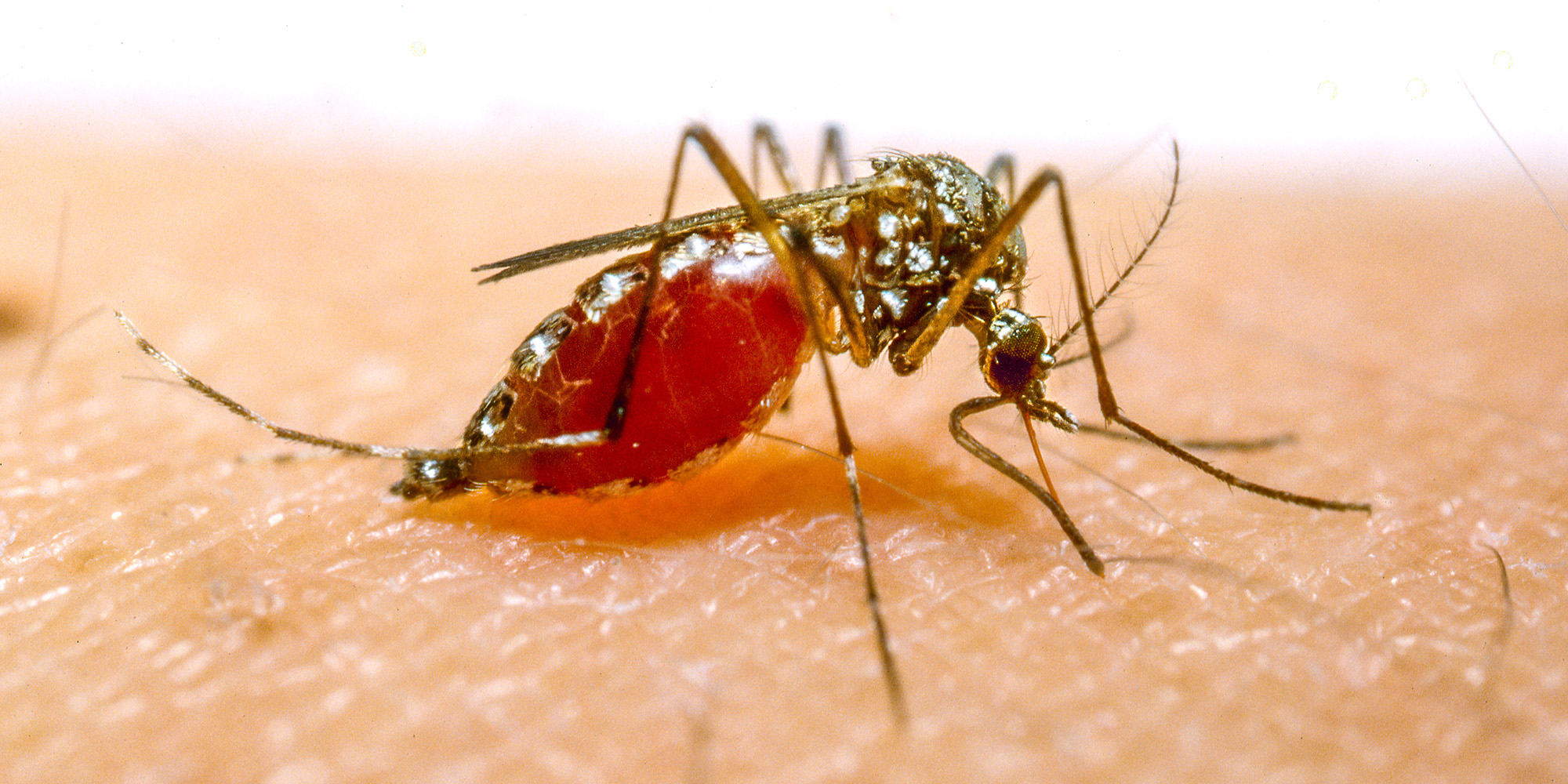
Weather Extremes Drive Increased Incidence of Infectious Diseases
With recent changes in weather toward warm and humid conditions as a result of changes in climate, infectious diseases that are spread to humans through nonhuman vectors are candidates for changes in their geographic location. These changes will potentially affect the ability of those vectors to survive, both increasing and decreasing areas of disease prevalence. To address these vectors and resulting emerging infectious diseases, it is necessary to utilize AI/ML and “team science” across a variety of areas like infectious disease surveillance, animal-human-plant health, ecology, and the environment. Five diseases that are intricately tied to the climate, the environment, animal reservoirs, and vectors include:
-

Sin Nombre virus – This hantavirus, spread directly from the deer mouse (P. maniculatus) to humans in contact with these mice or their excreta, causes hantavirus pulmonary syndrome (HPS); this is a rare but very serious disease, with a mortality rate of around 40 percent. In 1993, there was an HPS outbreak in the “Four Corners” region of the southwestern U.S. At the time, this was an “orphan” disease – a rare disease or condition that affects fewer than 200,000 people in the U.S. – but the “Hantavirus Study Group” quickly identified the virus and its vector. The relevance of this episode is that the reason for the outbreak was found to be a tenfold increase in the vector population triggered by an El Niño winter (heavy winter snow and spring runoff), leading to abundant vegetation and food for the mouse vector. This outbreak in 1993, which is a classic example of the link between climate and infectious disease, was also the first use of newly-developed PCR technology, applied to identifying an unknown infectious disease. Researchers continued to study the dynamics of the virus and environment in the Four Corners region for several decades. Public health officials now regularly use climate data to predict rodent populations and the resulting risks for hantavirus outbreaks.
-

Lyme disease and Powassan virus disease – Transmitted by the blacklegged tick (Ixodes scapularis) in the northeastern U.S. and upper midwestern U.S. and the western blacklegged tick (Ixodes pacificus) along the Pacific coast, Lyme disease is the foremost tick-borne disease in North America. A lesser-known disease, also spread by I. scapularis, is Powassan virus disease (POW), which was first isolated in Powassan ON, Canada, from a child who died from encephalitis. While Lyme is hardly trivial, POW is a very serious and often fatal neurological disease, with long-term neurological sequelae in survivors. Ixodes ticks spend most of the time out in the environment, and so are sensitive to its moisture content (they must not get desiccated). In addition, I. scapularis feeds on small rodents, which are also dependent on food availability and therefore the climate. Climate modeling studies in the U.S. predict future movement of I. scapularis westward and northward, leading to potential POW incidence increase in novel risk areas.
- Schistosomiasis – Second only to malaria as the most devastating parasitic disease, there is a potential impact of climate change on schistosomiasis transmission in China. Schistosoma japonicum is one of the three major schistosome species and causes schistosomiasis in that country. The parasite is spread to humans via contact with water in which an intermediate host snail, Oncomelania hupensis, has released sporocysts that develop into cercariae, the infectious form for humans. A research model based on forecasted temperature ranges in which the schistosome was able to develop within the snail predicted an expansion of schistosome transmission into currently non-endemic areas as a result of increased temperatures. Recently, an update was published that confirmed the earlier predictions for China, showing areas in which transmission would increase. At the same time, those same climate changes should decrease transmission in other areas in which disease is currently prevalent.
-

Malaria – The result of infection by Plasmodium species and transmitted by female Anopheles mosquitoes, six species of malaria are known to cause the disease in humans, among which P. vivax (SE Asia and western Pacific) and P. falciparum (Africa, SE Asia, and western Pacific) are the most dangerous. In 2020, the World Health Organization (WHO) estimated ~241 million cases globally, with 629,000 deaths; the majority of cases and deaths are in sub-Saharan Africa. Elimination of malaria worldwide is an ultimate objective for the WHO. The Plasmodium life cycle has an exogenous sexual phase (sporogony) which occurs in several species of Anopheles mosquitoes, and an endogenous asexual phase (schizogony) which takes place in the vertebrate host. Climate changes have diverse effects on the Plasmodium life cycle and other vectors such as Culex which causes West Nile Fever, since extreme temperatures, humidity, wind, and precipitation affect vector distribution and abundance. For example, increased precipitation will expand the mosquito distribution area and extend the length of transmission season. Currently, the number of human malaria infections in Eastern Africa, Nepal, and Colombia is rising, owing to warming of these regions, with an increase in competent malaria vectors favoring disease transmission at higher altitudes. Consequently, highland human populations that usually lack protective immunity are more vulnerable to severe malaria morbidity and mortality. Of course, although malaria transmission is climate-sensitive, like many other infections, it is a complex disease and changes in transmission cannot be attributed to climate alone.
- Valley fever – The common name for Coccidioidomycosis, Valley fever is a flu-like illness caused by a pathogenic fungus (Coccidioides spp). It is endemic in the southwestern United States and outbreaks often follow weather periods in which wet spells are followed by dry periods. The fungus grows in the wet period and spores that form when the land dries are easily spread through inhalation in dust clouds. A recent modeling analysis predicts, in a high-warming scenario, that the disease will become endemic in an additional five states in the Western North U.S., with cases jumping by 50 percent by 2100. Whether all of this will come to pass is uncertain, but the disease has recently spread to south central Washington state, and, with warming continuing through this century, at least some of this scenario seems likely to occur. In another nod to climate effects, a tsunami has also been suggested as a cause for the spread of this disease.
While the multifaceted effects of climate change are complex, one of them is believed to be the increased incidence of infectious diseases. A team science approach is necessary to help mitigate the threat.
GETTING STARTED AT MRIGLOBAL
Contact MRIGlobal for further information about our work with infectious diseases. Through an interdisciplinary approach, we provide scientific and subject matter expertise for development of research against such disease threats, while expanding and accelerating the delivery of high quality clinical diagnostic products.
To discuss how we can help your project be successful, contact us today.
SIGN UP FOR OUR NEWSLETTER
Sign up for the MRIGlobal newsletter! It’s the best way to get the latest updates in the world of applied scientific engineering research delivered directly to your inbox.